Patients with achalasia in the GP surgery
By John Galloway FRCP, Specialist GP in GI Medicine (Retired)
Achalasia is a rare and benign neurodegenerative disorder characterised by failure of relaxation of the lower oesophageal sphincter and loss of peristalsis in the distal oesophagus. The aetiology is unknown although there may be an autoimmune component. A patient presenting in a GP surgery with achalasia is rare (incidence approx. 0.7 – 1.6 per 100,000; prevalence 3-4 in 1 million). Achalasia typically occurs in adults aged 25-60 years. The male-to-female ratio is 1:1 and less than 5% of cases occur in children.
Patients are likely to present with dysphagia (most common) often with regurgitation, chest pain, heartburn and weight loss.
Since all pathology beyond the fauces relating to swallowing is inaccessible to physical examination, most useful information is obtained from a carefully taken history to discover whether the patient really has dysphagia and where the cause is likely to be situated. Dysphagia is a symptom to be taken seriously and merits investigation unless the cause is obvious such as acute tonsillitis.
Differential diagnosis of dysphagia, listed below, can be divided into:
- Pharyngeal
- Stricturing lesions of the oesophagus
- Extrinsic Causes
- Acute onset
- And, most relevant to achalasia, motility disorders of the oesophagus.
Signs and Symptoms particularly relevant for achalasia
- Food getting stuck in the chest area near or above the diaphragm
- Regurgitation of undigested food, as distinct from vomiting from stomach
- Sometimes, painful chest spasms
- Sometimes, breath smelling from food accumulated in oesophagus
- A need to distinguish achalasia from eating disorders. The process of eating and its consequences may well cause tension and anxiety, rather than a psychological issue creating a desire not to eat.
- Particular problems with food with difficult textures likely to cause a blockage at the lower oesophageal sphincter or which may congeal (eg tomato skins, grapes, rice, white bread)
- Relief from symptoms if patient stands up, drops on to heels or otherwise physically dislodges a blockage.
- Sometimes, candidiasis potentially originating in the oesophagus
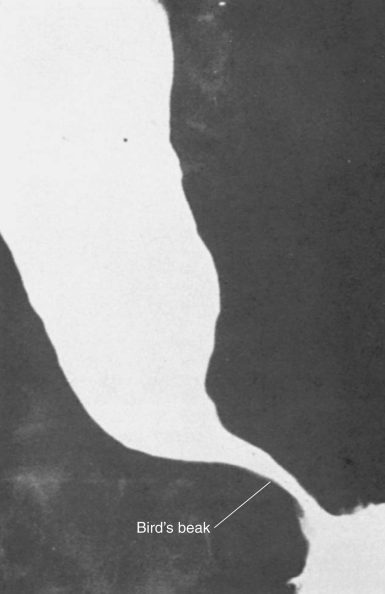
Achalasia can only be properly diagnosed after endoscopy, barium meal swallow test and manometry. Endoscopy may well appear normal in achalasia, but food residue and a dilated oesophagus may be relevant and noted. If symptoms persist after a normal endoscopy with negative histology to rule out eosinophilic oesophagitis, it may be appropriate to make a referral for a barium swallow test (where a distorted oesophagus and narrowed lower oesophageal sphincter and dilatation above give the “bird’s beak” appearance) if this has not already been undertaken in specialist care.
Differential Diagnosis of Dysphagia
- Pharyngeal Causes
- Tonsillitis
- Muscular dystrophy
- Myasthenia gravis
- Polymyositis, dermatomyositis
- Brainstem CVA
- Parkinson’s disease
- Motor neurone disease
- Multiple sclerosis
- Mucosal webs
- Carcinoma/ pharynx/larynx
- Pharyngeal pouch
- Stricturing lesions of the oesophagus
- Peptic stricture /erosive oesophagitis
- Caustic stricture caused by ingestion of caustic or hot substances
- Carcinoma
- Shatski ring
- Motility disorders of oesophagus
- Achalasia
- Diffuse spasm
- Scleroderma Eosinophilic oesophagitis (caused by cellular infiltration of the oesophagus and stiffening of the structure)
- Extrinsic causes
- Carcinoma of the bronchus
- Retrosternal goitre
- Aortic arch lesions
- Mitral stenosis- giant left atrium
- Acute onset
- Impaction of foreign body
- Impaction of food bolus
- Candida infection of oesophagus
- Acute ulceration – drug induced
- Intramural haematoma
- Radiotherapy to mediastinum